The Science of Spinal Decompression: Biomechanical Restoration
- parkerneilldc
- Apr 5
- 3 min read
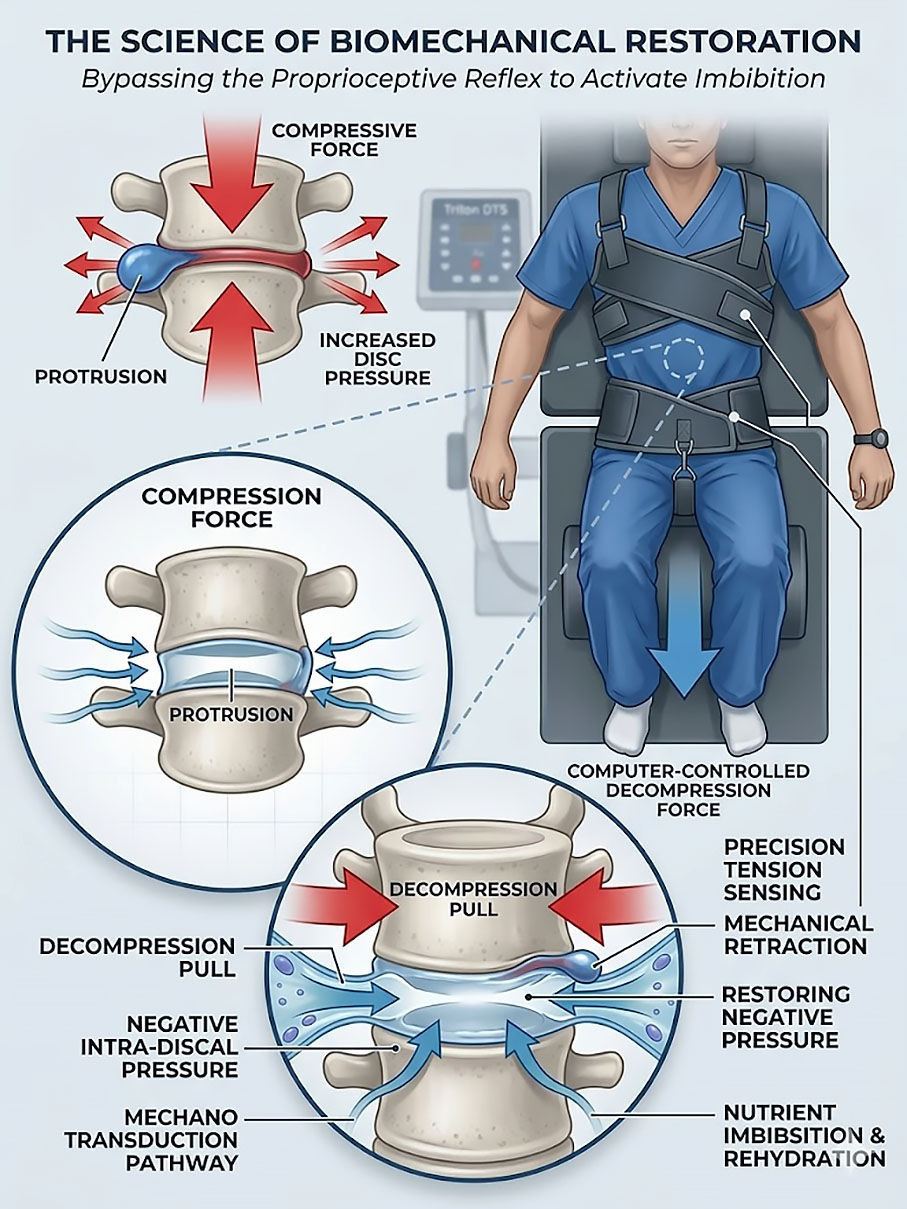
In the field of advanced spinal care, there is a profound distinction between simply stretching the back and understanding the science of spinal decompression to achieve true neuromusculoskeletal restoration. For high-information patients—particularly the engineering and research professionals throughout Cary and the Research Triangle—understanding the mechanical and physiological "why" behind a treatment is essential for making informed healthcare decisions.
Traditional methods often fall short because they fail to account for the body’s innate neurological defenses. To understand why computerized spinal decompression is a clinical advancement, we must look at the intersection of physics, neurology, and cellular biology.
The Physics of Negative Intra-Discal Pressure
The human intervertebral disc is a pressurized, fluid-filled structure. Under normal conditions, it acts as a primary shock absorber for the spine. However, due to chronic "static loading"—common in sedentary professional roles—or acute trauma, these discs can lose height and the ability to hydrate, leading to protrusions or herniations.
Non-surgical decompression utilizes a specific logarithmic pull-pattern to create negative intra-discal pressure. While traditional traction applies a linear, "dumb" force that can cause the disc to resist, computerized decompression creates a vacuum effect. This vacuum—measured in millimeters of mercury (mmHg)—serves two primary clinical purposes:
Mechanical Retraction: It creates a centripetal force that encourages displaced nuclear material to move back toward the center of the disc.
Nutrient Shunting (Imbibition): It facilitates the intake of oxygen, water, and nutrients into the disc space, which is a requirement for tissue repair.
The Science of Spinal Decompression: Bypassing the Proprioceptive Reflex
The greatest challenge in spinal mechanical therapy is the proprioceptive reflex. The human body is equipped with sensory receptors called Golgi tendon organs and muscle spindles that monitor tension.
When a standard traction device or an inversion table pulls on the spine, these sensors detect the stretch as a potential threat. In response, the nervous system triggers a "guarding" reflex, causing the paraspinal muscles to contract to protect the spine. This contraction actually increases the pressure on the disc, defeating the purpose of the treatment.
The sophistication of computerized decompression lies in its ability to bypass this reflex. The system’s sensors monitor muscle resistance thousands of times per second. If the system detects the slightest hint of muscle guarding, it instantly adjusts the tension. By "whispering" to the nervous system rather than shouting at it, the technology allows the paraspinal muscles to remain relaxed, ensuring the force reaches the intended deep-tissue structures.
Mechanotransduction: Repair at the Cellular Level
The clinical goal of decompression extends beyond immediate pain relief; it aims for biomechanical restoration. This is achieved through a biological process called mechanotransduction.
Mechanotransduction is the mechanism by which cells convert mechanical stimulus into biochemical activity. When the disc is subjected to the specific cycles of loading and unloading provided by a computerized system, it signals the fibroblasts and chondrocytes within the disc to increase the production of collagen and proteoglycans.
In simpler terms, the mechanical pull actually commands the disc to begin repairing its own structural integrity. This is why decompression is categorized as a "functional" treatment rather than a temporary "fix."
Establishing Clinical Candidacy
Not every patient with back pain is a candidate for decompression. High-authority care requires a rigorous clinical evaluation to assess the neuromusculoskeletal system as a whole. This involves analyzing:
Segmental Mobility: Identifying which specific levels of the spine are restricted or dysfunctional.
Neurological Integrity: Assessing dermatomes and myotomes to ensure the nerve pathway is viable for recovery.
Biomechanical Load: Evaluating how a patient’s daily activities contribute to ongoing disc desiccation.
A Foundation for Physical Resilience
By moving away from outdated models of "alignment" and focusing on the hard science of biomechanical restoration, patients can transition from chronic management to long-term physical resilience. Computerized spinal decompression represents the pinnacle of non-surgical intervention, merging the precision of modern engineering with the complexities of human physiology.




Comments